Current echocardiographic assessment of the aortic bioprosthesis showed calcified neo-cusps with reduced systolic opening and a mean systolic pressure gradient of 27 mmHg (corrected for V1 in the left ventricular outflow tract), a maximum systolic flow velocity of 3.4 m/s, a dimensionless index of 0.30, and a calculated effective orifice area (EOA) of 1.1 cm
2 (0.6 cm
2/m
2) from the apical 5 chamber view (
fig. 1A and B) [
1]. As maximum flow velocities occurring due to aortic stenosis are expected distal of the anatomic orifice, this first imaging window was considered inappropriate, because no colour Doppler signal in the region of the sinus portion could be detected (
fig. 1A, circle). After careful re-alignment of the transducer, slightly better visualisation of blood flow distal of the aortic valve was achieved, and a maximum flow velocity of 3.8 m/s could be measured (
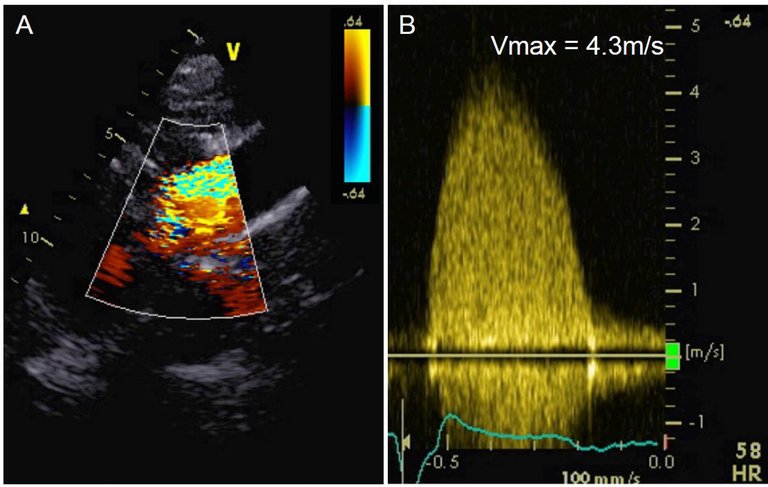
fig. 1C and D; circle in C indicating visualisation of flow distal of the prosthesis using colour Doppler imaging). We suspected that maximum flow velocity was still underestimated owing to profound ultrasound attenuation in the area distal to the valve when acquiring Doppler signals from an apical transducer position as a result of severe degenerative alterations of the bioprosthetic valve. Therefore, we re-assessed the transvalvular pressure gradient from a right suprasternal position with the patient in a right lateral position. This manoeuvre revealed a mean systolic transvalvular pressure gradient of 43 mmHg with a more parabolic shape of the Doppler spectrum, maximum flow velocity 4.3 m/s, dimensionless index 0.15, and calculated EOA 0.6 cm
2 (0.3 cm
2/m
2);
fig. 2). These findings proved the existence of a severe stenosis of the aortic prosthesis and provided a reasonable explanation for the patient’s complaints.